All-Payer Patient Insurance Verification
About Us
All-Payer Patient Insurance Verification Leader with Real-time, API, and Batch Solutions showcasing comprehensive Patient Eligibility and a suite of solutions for Medicare, Medicaid, Commercial, Dental, and Vision Payers.
All-payer Patient Insurance Verification
The Journey Started
pVerify® was founded in 2006 by a team of accomplished Healthcare Professionals with a singular focus: streamline the front-end patient insurance eligibility and benefit verification processes in order to not only improve patient collections but also reduce back-office denials.
Powered by its own APIs pVerify aimed it’s focus on studying over 1350 payer responses to compile unique eligibility settings for each. Championing the highest level of benefits parsing with consumable API endpoints, pVerify’s team of expert developers stride forward to refine and maximize benefit reporting.
Our unique blended process allows us to delivery the most pertinent patient eligibility information across all payers – even if the payer 270/271 report doesn’t include all of the required elements or even if the payer does not support EDI 270/271. Then, unlike other services, we provide verified patient benefits at a deeper level, with information separated and highlighted individually for easier review and understanding . For our First-Class Batch we present the results in a color-coded Microsoft Excel spread-sheet format so that a front-office, verification team, or billing staff can collect appropriate patient payments and spot inaccuracies relating to patient demographics or insurance information.

In the industry of Eligibility vendors, pVerify shines with 15 years of historic medical verification knowledge and innovative technological capabilities to help world-class developers build comprehensive verification systems beyond the average 270/271. We understand unique responses from individual payers and guide from pre- to post-development, allowing for more information to be captured, parsed, and returned in every API Call and Premium Portal Verification.
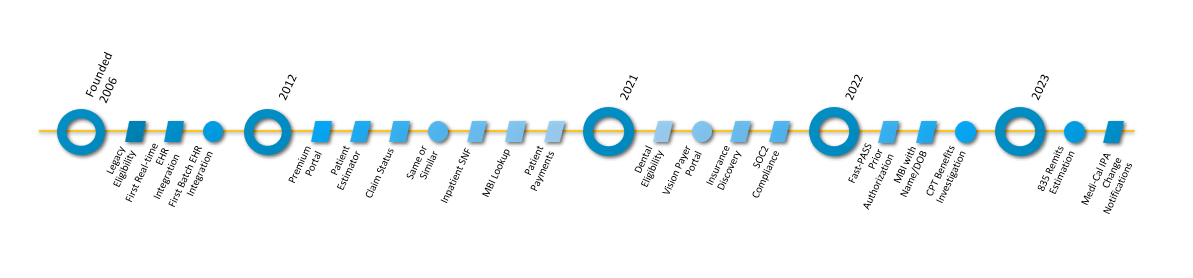
A Brief Timeline of pVerify, Inc
Meet The Team
Have a question?
Please fill out our Contact Form and a pVerify Representative will contact you within 24hrs.
Request more information
Complete the fields below.
How Can We Help You?
Get answers before you subscribe.
All-Payer Patient Insurance Verification and MORE!
Our automated, date-of-service patient insurance verification brings unprecedented efficiency to your front-office workflow. Coupled with our Patient Estimator and hands-free Patient Payment, our Solutions can significantly reduce patient debt and improve front-office collections. Supported in Realtime, Batch, and API
Advanced Eligibility
Large Medical Provider Solutions
Next-level Customization with Business Rule Knowledge Base and Expert Consulting Services